CLIAwaived, Inc 7 Panel - IDTC II
(25 Cups)
| New Tiered Pricing | Quantity Required | Price per Box |
| Tier 1 | 1 - 11 Boxes | $87.50 per Box |
| Tier 2 | 12 - 32 Boxes | $81.25 per Box |
| Tier 3 | 40+ Boxes | $74.75 per Box |
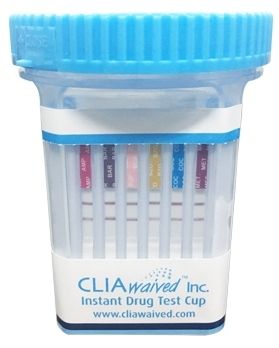
CLIAwaived, Inc. - INSTANT DRUG TEST CUP/CARD II (IDTC II). This 7-panel, no-leak drug test cup tests for BZO, COC, MET, MTD, THC, OPI (MOR 300) and OXY. Results in 5 minutes.
FDA-cleared and CLIA-waived.
To Recieve Certificate on Product Please Review Training found in Product Attachements. Once reviewed you can click on the link right below to take our training quiz and be emailed your Certificate.
(IDTC II) TRAINING QUIZ (cliawaived.com)
Ground Shipping only! To get a shipping quote for expedited delivery please call (888)882.7739.
FEATURES:
- Fast, dark test lines
- Negative results visible within one minute
- Non-negative results in five minutes
- Donor-friendly cup opening
- Results can be photocopied
- Remarkable pricing and quality
- FDA-cleared and CLIA-waived
CLIAwaived, Inc. IDTC CUPS WILL DETECT FROM 5 - 12 DRUGS: NOT ALL CUPS DETECT ALL DRUGS LISTED BELOW
- Amphetamine (AMP)
- Barbiturates (BAR)
- Buprenorphine (BUP)
- Benzodiazepines (BZO)
- Cocaine (COC)
- Ecstasy (MDMA)
- Methadone (MTD)
- Methamphetamine (MET)
- Marijuana (THC)
- Opiates 300 (OPI 300)
- Oxycodone (OXY)
- Phencyclidine (PCP)
- Tricyclic Antidepressants (TCA)
+ 3 ADULTERANTS (CRE, SG, OX)
CPT Code*: 80305QW - Drug test(s), presumptive, any number of drug classes, qualitative; any number of devices or procedures, (e.g., immunoassay) capable of being read by direct optical observation only (e.g., dipstick, cups, cards, cartridges) includes sample validation when performed, per date of service (maps to 80300 or G0477).
National Average Reimbursement 2019: $12.60
*All CPT codes are supplied for information purposes only and represent no statement; promise or guarantee by CLIAwaived Inc. that these codes will be appropriate or that reimbursement will be made. It is the responsibility of the service provider to confirm the appropriate coding required by their local Medicare carriers, fiscal intermediaries and commercial payors.