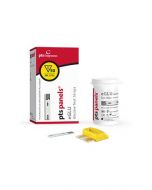
CHOL+GLU Test Strips
(25 Tests)
| New Tiered Pricing | Quantity Required | Price per Box |
| Tier 1 | 1 - 3 Boxes | $117.84 per Box |
| Tier 2 | 4 - 9 Boxes | $110.48 per Box |
| Tier 3 | 10+ Boxes | $107.78 per Box |
PTS Panels CHOL+GLU Test Panel test strips are intended to measure cholesterol and glucose in whole blood on a CardioChek PA Analyzer. (Note: Select part #CHEK-2865 or ST-1040-15 for blood collection.)
FDA-cleared and CLIA-waived. (FDA 510K#: K041750) FOR PROFESSIONAL USE ONLY. CALL FOR DISCOUNTS AND VOLUME PRICING!
PTS Panels CHOL+GLU Test Panel test strips measure total cholesterol, and glucose in whole blood with the CardioChek PA Analyzer. The test strips are intended to measure cholesterol and glucose in whole blood. Cholesterol measurements are used in the diagnosis and treatment of disorders involving excess cholesterol in the blood and lipid and lipoprotein metabolism disorders. Glucose measurements are used in the management of carbohydrate metabolism disorders.
A MEMo Chip is provided with each package of test strips, and must be properly inserted into the analyzer before any test an be run. The MEMo Chip contains the test name, calibration curve, lot number and test strip expiration date. After the test strip is inserted into the analyzer and blood applied to the strip, test results are displayed in about a minute.
BENEFITS:
- Fast turn-around time with results in minutes
- Easy operation
- Long shelf-life with no refrigeration requirements
- Accurate results
Materials provided:
- PTS Panels Cholesterol Test Strips
- MEMo Chip (contains lot-specific test strip information)
- Instructions
NOTE: FOR PROFESSIONAL USE ONLY. For use only with the CardioChek PA Test Systems.
CPT Code*
- 82465QW - Cholesterol, Serum or whole blood, total
- National Average Reimbursement 2019: $4.84
- 82947QW - Glucose; quantitative, blood (except reagent strip)
- National Average Reimbursement 2019: $4.37
*All CPT codes are supplied for information purposes only and represent no statement; promise or guarantee by CLIAwaivedTM Inc. that these codes will be appropriate or that reimbursement will be made. It is the responsibility of the service provider to confirm the appropriate coding required by their local Medicare carriers, fiscal intermediaries and commercial payors.